Picture this: it’s late on a Tuesday night, your chest starts to hurt, and the nearest urgent care is a 45-minute drive down a dark, winding mountain road. No ambulance is close by. No walk-in clinic down the street. Just you, your car, and the hope that nothing gets worse before you get there. For millions of Americans living in the rural Northwest, this is not a worst-case scenario – it’s a Tuesday. The healthcare desert crisis in the United States has grown quietly for decades, and the warning signs are now impossible to ignore. Let’s dive in.
1. The Scale of the Problem: Over 100 Million Americans in Shortage Zones

The number of federally designated primary care healthcare professional shortage areas has actually declined since 2021, but this is largely due to a system reclassification that withdrew shortage designations in 2024 for many facilities, not because primary care shortages actually improved. Let that sink in. The problem didn’t get smaller. The measuring stick just moved.
The average patient caseload in remaining federally designated primary care deserts, home to nearly 8 million people, is still one full-time primary care professional for every 7,597 people. That’s more than two and a half times the recommended level. The gap between supply and demand isn’t closing anytime soon.
2. The Northwest Is Uniquely Vulnerable
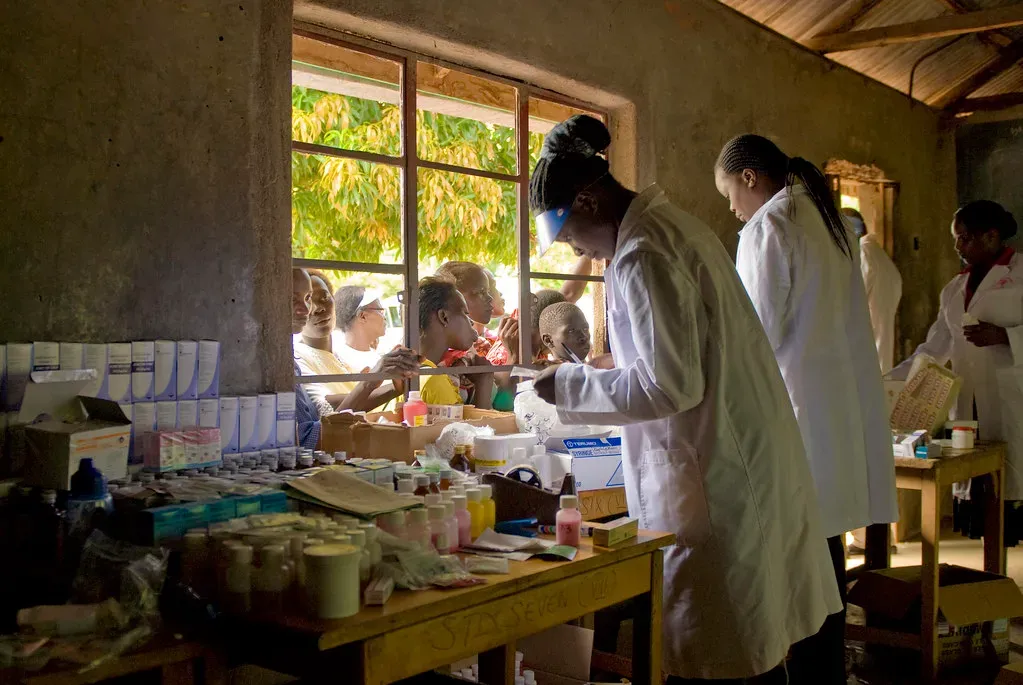
The wide-open landscapes of Idaho, Montana, Washington, and Oregon are breathtaking – and brutally isolating when you need medical care fast. Montana, North Dakota, Wyoming, Nevada, and Idaho currently have the most trauma desert counties, and in these states, the majority of residents will not be able to access a trauma center within the “golden hour.”
Healthgrades found that residents in rural states including Idaho remain disproportionately affected by lack of access to high-quality care. Honestly, when geography itself becomes a health risk factor, you know the system has a serious structural problem on its hands.
3. Rural Hospitals Are Closing at an Alarming Rate

Between 2005 and 2023, 146 hospitals in rural U.S. counties closed or were converted to non-acute care. Of those, 81 shut down completely. Think of it like a slow landslide. Each closure quietly reshapes the landscape of care, and communities often don’t feel the full weight of it until there’s an emergency.
Although the number of rural hospital closures and conversions slowed in certain years, it started to rise again after 2022. Financial stress is the primary driver, with contributing factors including smaller size, lower occupancy rates, and greater vulnerability to economic fluctuations than urban hospitals.
4. Hundreds More Hospitals Are on the Brink
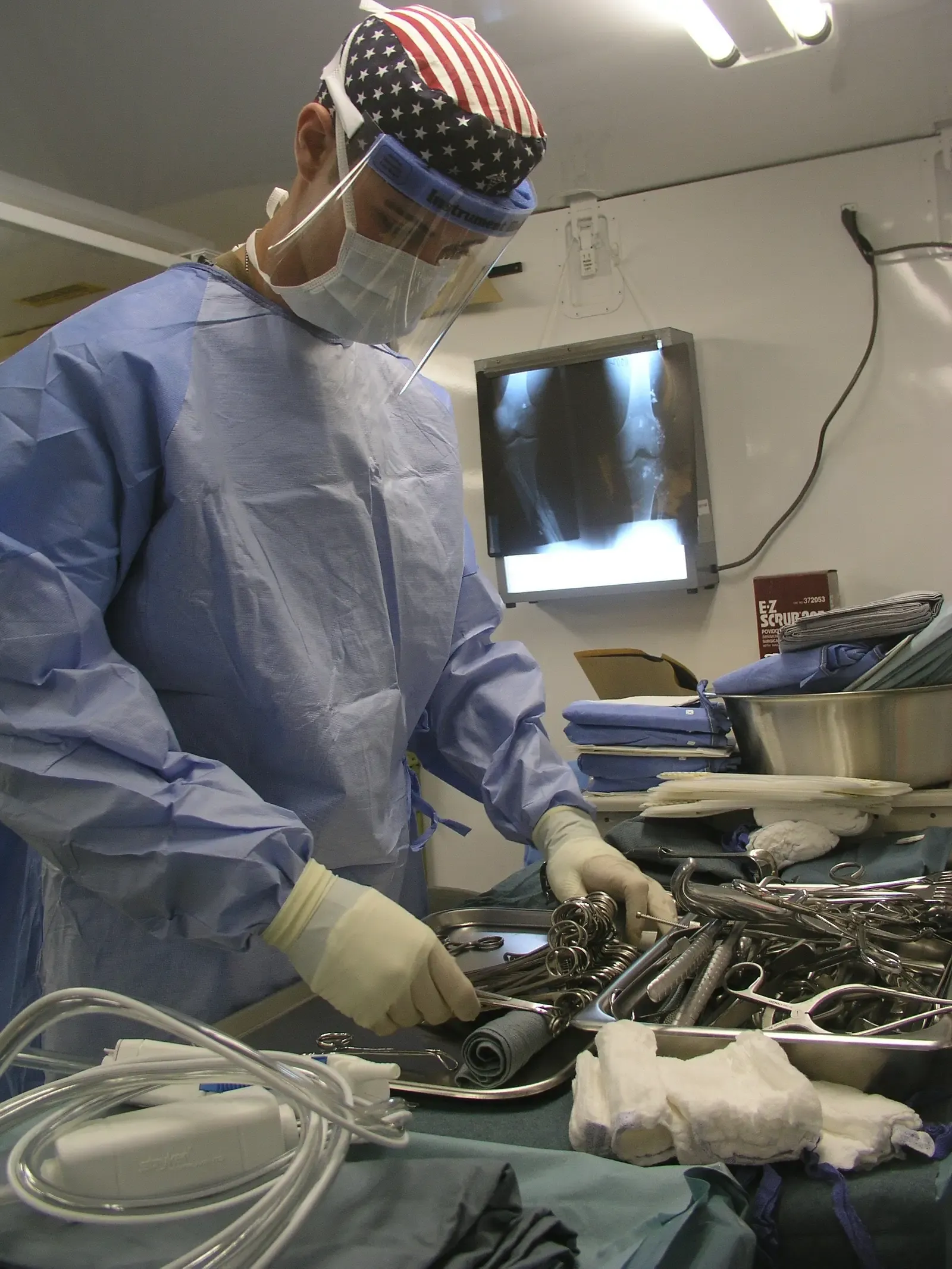
The closures that have already happened are troubling enough. What’s coming next is alarming. According to a March 2025 report, more than 768 rural hospitals are currently at risk of closing, with 315 of them imminently. That’s not a slow trickle anymore. That’s a flood approaching the dam.
Residents in remote areas of the U.S. face increasing barriers to critical health services, with more than 200 rural hospitals completely or partially closing since 2005 and 400 more currently at risk of closure. The Commonwealth Fund has also flagged that changes to national health policy, including Medicaid adjustments, are expected to make things worse, not better.
5. The Physician Shortage Is Getting Worse, Not Better
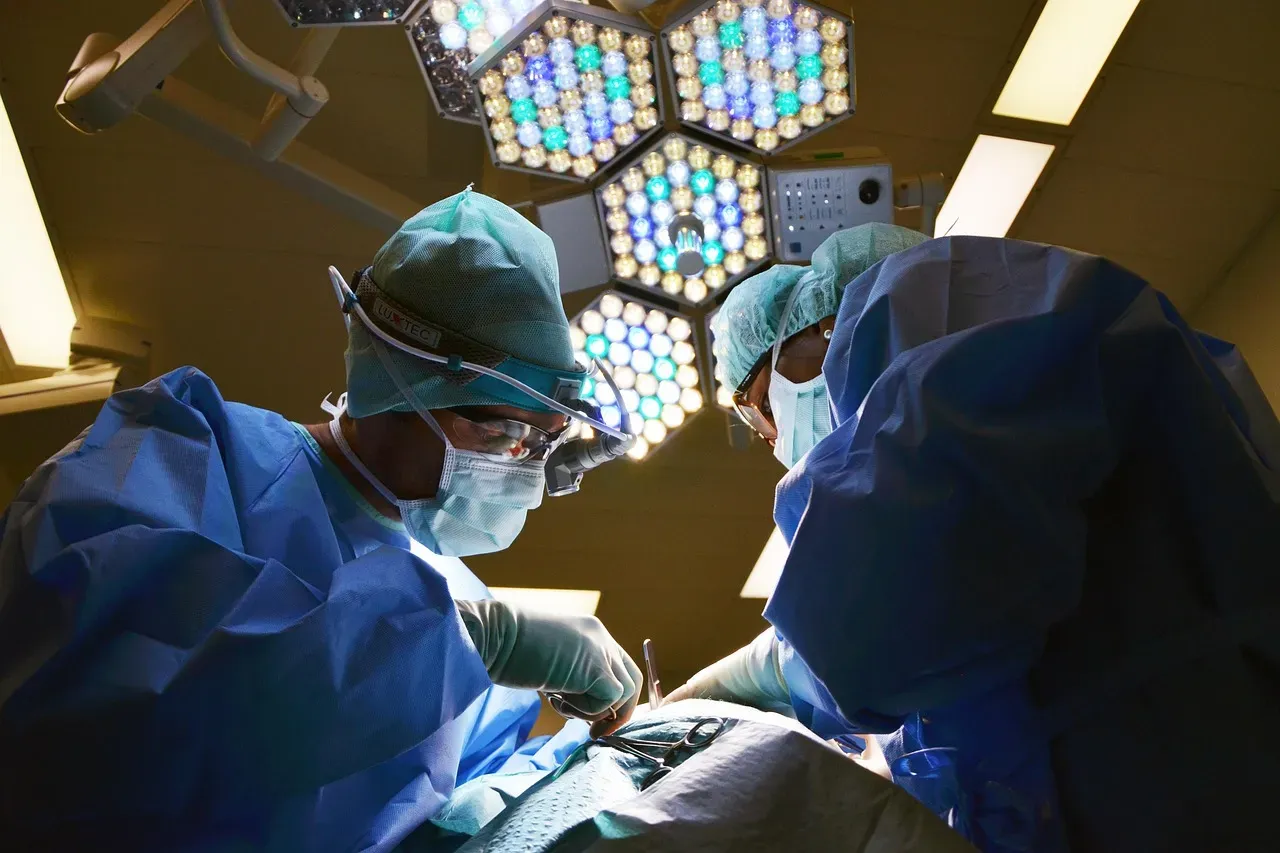
Here’s the thing: even if you keep the hospital building open, it doesn’t mean much without the doctors inside it. The United States is facing a nationwide healthcare worker shortage, and in rural communities, this crisis is worse and more widespread. According to calculations by the Joint Economic Committee, roughly 91% of all rural counties face a shortage of primary care physicians.
Studies have found that medical professionals who were raised in rural areas are far more likely to practice in rural areas than their urban peers. However, students from rural backgrounds make up under 5% of the incoming medical student body. That gap between background and opportunity is, in many ways, the root of the whole problem.
6. Montana’s Landscape Makes Everything Harder

In Montana, the vast and sparsely populated landscape presents additional challenges for rural healthcare. The closure of a single hospital can mean that residents must travel farther distances for basic healthcare services, a situation exacerbated by counties that no longer have ambulatory services. This not only affects the timely delivery of care but also increases demand on surrounding healthcare facilities.
While Montana has expanded Medicaid, recent redetermination of Medicaid benefits eligibility post-COVID disenrolled nearly 93,000 Montanans. That’s nearly 93,000 people who slipped back into uncertainty. Progress is fragile when one policy shift can undo years of gains.
7. The Ripple Effect on Maternity and Obstetric Care

It’s not just emergency rooms and primary care that are disappearing. Maternity care is quietly vanishing from rural communities too. Between 2011 and 2023, 293 rural hospitals stopped providing obstetric services, representing roughly a quarter of the nation’s rural OB units. Rural OB deserts now stretch across vast stretches of rural America and heighten the stakes in the event of a medical emergency.
For rural patients, the average travel time to the nearest hospital with birthing services jumps to 26 minutes, and for maternity care desert residents, it can extend up to 38 minutes. The highest travel times were found in Alaska, West Virginia, Wyoming, Hawaii, and Montana. For a woman in active labor, that 38-minute drive isn’t just inconvenient. It’s potentially life-threatening.
8. Rural Residents Pay With Their Health

Distance from care isn’t just logistically frustrating. It translates directly into worse health outcomes. People who live in rural areas of the United States are more likely than urban residents to die prematurely from chronic diseases. These rural residents are more likely to die prematurely from five of the leading causes of death: heart disease, cancer, stroke, unintentional injuries, and chronic lower respiratory disease.
When a rural hospital closes, patients may have to travel further to obtain services, which could lead some to forgo care altogether. Closures may be especially problematic for people who have difficulty traveling long distances and for people with time-sensitive conditions, such as heart attacks and childbirth. In healthcare, delayed care is often no care at all.
9. Telehealth Promised Relief, But Broadband Gaps Remain

Telehealth was supposed to be the great equalizer. To a degree, it surged powerfully during the pandemic. Medicare telehealth visits exploded from roughly 840,000 in 2019 to more than 52 million in 2020, according to the U.S. Department of Health and Human Services. That’s not a trend – that’s a revolution in a single year.
Healthcare access suffers significantly in rural locations where broadband infrastructure is lacking, due to limited telehealth services and delayed care. Rural communities lack simple access to healthcare because of the almost impossible use of telemedicine services without broadband. Delayed care can adversely impair the health outcomes of patients in rural areas, often due to extended travel times and delays in diagnosis and treatment. The digital divide and the healthcare desert often overlap like a Venn diagram of disadvantage.
10. The Northwest Is Starting to Fight Back

It would be easy to end this article on a note of despair. The numbers are genuinely sobering. Yet there are real efforts underway, and some of them are promising. The University of Washington School of Medicine’s Rural Underserved Opportunities Program serves underserved rural counties and boroughs across Washington, Wyoming, Alaska, Montana, and Idaho, offering a four-week rotation for students between their first and second years of medical school. The idea is simple but powerful: if you show young doctors rural medicine early, they may actually choose it.
State-level initiatives, such as the organization of tax districts in Washington and Iowa, have helped to ease the financial burden for rural hospitals and support maintaining access to care. By leveraging technology, patients in rural areas can receive consultations and care from specialists located elsewhere, reducing the need for travel. Community-driven initiatives and alternative funding models are also being explored to sustain rural healthcare, including community health partnerships and localized health programs tailored to the specific needs of rural populations. None of this is a silver bullet, but it represents real, local momentum.
Conclusion: The Road Is Too Long

A 45-minute drive for urgent care might sound manageable to someone in a city. But pair that drive with a winter snowstorm, a failing vehicle, a medical emergency in the middle of the night, or a family without reliable transportation, and it becomes something far more serious. The loss and potential future loss of access to care is compounded by rural America’s weakening population health status and expanding care deserts for vital services. For the more than 46 million people who live in rural areas, the rapid deterioration of access to care raises pointed questions about the safety net’s ability to continue to meet the needs of these communities.
Healthcare deserts are not a natural disaster. They are the accumulated result of funding shortfalls, policy gaps, workforce pipelines that never quite reached remote places, and decades of decisions made mostly in cities. The Northwest is beautiful. Its residents deserve not to have to gamble with their lives every time they get sick. What do you think needs to change first? Tell us in the comments.