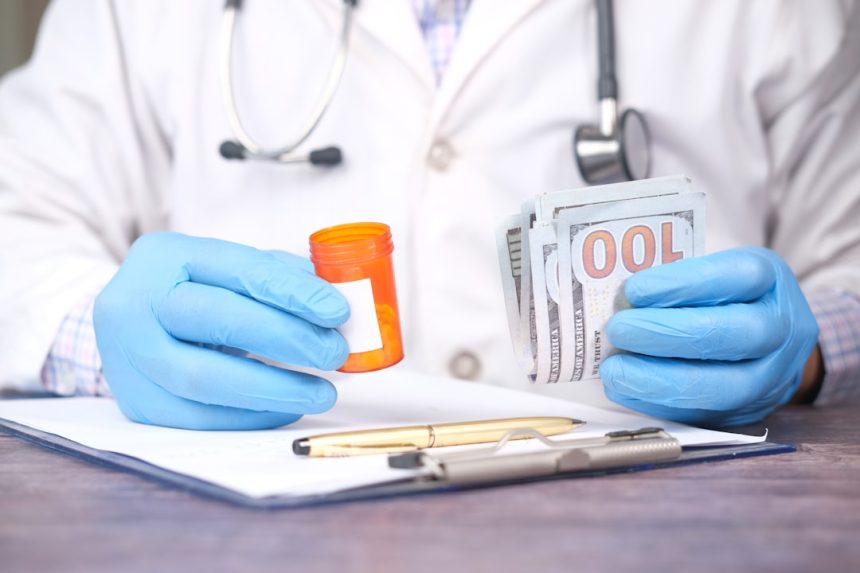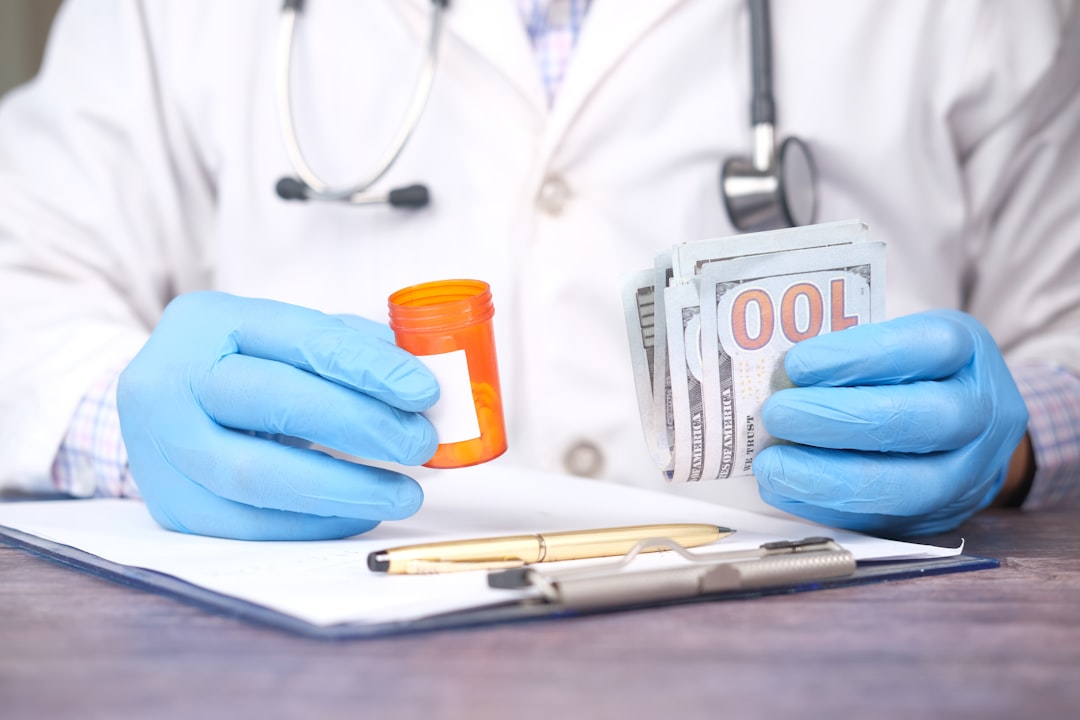
Spotting the Red Flags in Your Medicare Statements (Image Credits: Unsplash)
Las Vegas – Medicare fraud drains an estimated $60 billion annually from the program, affecting beneficiaries nationwide including those in Nevada.[1] Recent cases in the area, such as a local nurse practitioner pleading guilty to fraudulent billing, highlight the risks close to home.[2] Government resources urge quick reporting of suspicious claims to protect personal benefits and halt scammers.
Spotting the Red Flags in Your Medicare Statements
Beneficiaries receive a Medicare Summary Notice every three months for Original Medicare, detailing services, charges, and payments. Online accounts at Medicare.gov provide monthly access to claims, allowing earlier detection. Unfamiliar services, incorrect dates, or charges for items never received signal potential fraud.
Common scams involve billing for unprovided tests, genetic screenings, or durable medical equipment like braces. Providers sometimes use wrong diagnoses to justify payments. Local incidents in Las Vegas have included schemes targeting wound care and hospice services, underscoring the need for vigilance.[3]
First Steps When You Notice a Suspicious Charge
Contact the listed provider immediately to verify the claim. Many errors stem from billing mistakes rather than intentional fraud. Gather your records, including appointment calendars and receipts, to compare against the statement.
Access your secure Medicare account to review full claim details. If the provider cannot explain the charge, escalate promptly. Avoid paying any disputed amounts yourself, as Medicare handles adjustments.
Reporting Fraud: Key Contacts and Processes
Call 1-800-MEDICARE at 1-800-633-4227 to report suspicions, available for Original Medicare issues.[4] Provide your Medicare number, provider details, service dates, and why the claim seems wrong. For Medicare Advantage or drug plans, reach the Investigations Medicare Drug Integrity Contractor at 1-877-7SAFERX (1-877-772-3379).
File reports online via the Medicare fraud reporting page or the HHS Office of Inspector General at 1-800-HHS-TIPS (1-800-447-8477) or tips.oig.hhs.gov.[4] Have evidence ready, such as the Medicare Summary Notice or claim ID.
Preventive Measures to Safeguard Your Benefits
Treat your Medicare card like cash; share your number only with trusted doctors or providers. Medicare never requests it unsolicited via phone, email, or door-to-door visits. Record all medical appointments and cross-check against statements monthly.
- Decline free offers requiring your Medicare number.
- Question providers about billing practices and copays.
- Verify prescriptions and supplies match your doctor’s orders.
- Avoid unsolicited medical equipment deliveries.
- Hang up on callers demanding personal information.
These habits reduce risks of identity theft and improper billing.[5]
Local Support: Nevada’s Senior Medicare Patrol
Nevada’s Senior Medicare Patrol offers free assistance for fraud detection and reporting. Contact LaDonne Knighten at (702) 486-6355 or lknighten@adsd.nv.gov for Las Vegas-area help.[6] The program educates on protecting information and spotting errors.
State resources complement national hotlines, providing personalized guidance. Recent enforcement actions in Nevada demonstrate authorities’ commitment to cracking down on schemes.[2]
Key Takeaways
- Review statements regularly via mail or online account.
- Report suspicions immediately to 1-800-MEDICARE.
- Leverage local SMP for Nevada-specific support.
Swift action preserves Medicare’s integrity and your financial security. Staying proactive shields benefits from thieves. What steps will you take to check your latest statement? Share in the comments.