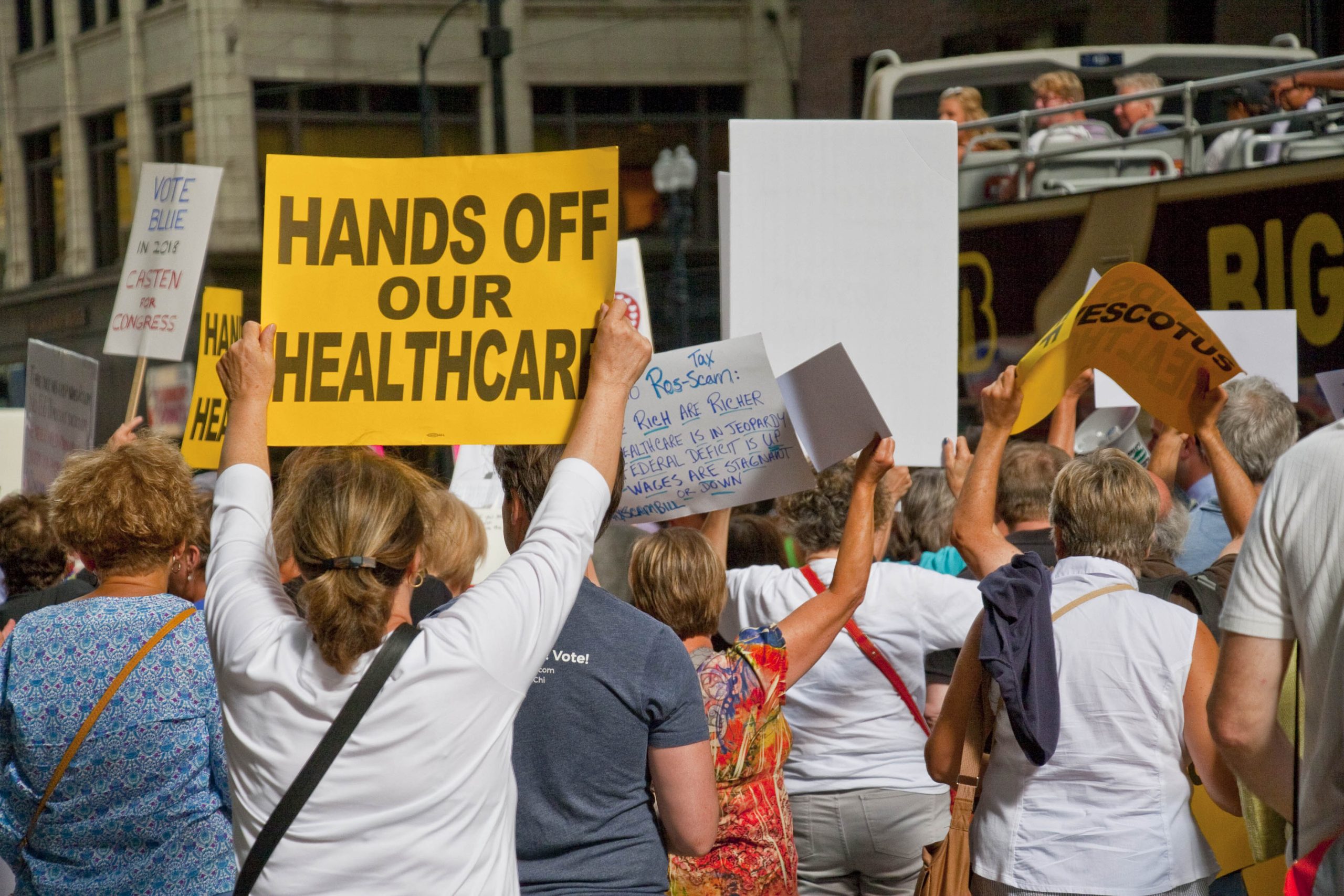
Heightened Fears Fueled Political Drama (Image Credits: Upload.wikimedia.org)
Washington – Democrats had predicted catastrophe when enhanced Affordable Care Act subsidies expired at the end of 2025. Lawmakers warned of soaring premiums and millions dropping coverage, even triggering a prolonged government shutdown to demand an extension. Yet four months into 2026, federal data reveals no such collapse occurred. Enrollment dipped modestly, and costs for most subsidized users stayed manageable.
Heightened Fears Fueled Political Drama
Senate Democrats initiated a government shutdown from October 1 to November 12, 2025 – the longest in U.S. history – to compel Republicans to renew the temporary subsidies introduced during the COVID-19 pandemic.[1]
They portrayed the expiration as a Republican plot to dismantle healthcare access. One Democratic representative blamed House Republicans directly for impending “skyrocketing health care costs.”[1] Political outlets noted Democrats eyed the issue as a potent midterm attack line.
Advocates projected premium doublings and coverage losses for 22 million people nationwide. In Nevada, state marketplace enrollment concerns mirrored national anxieties, with early reports of potential dips amid rate hikes.[2]
What the Numbers Actually Show
The Centers for Medicare and Medicaid Services released enrollment figures that defied the gloom. Plan selections for 2026 totaled 23.1 million, down from a record 24.3 million the prior year but well above 16.3 million in 2024.[1][3]
Nevada Health Link reported a nearly 6 percent decline in enrollments for 2026 coverage, yet numbers held relatively steady compared to projections.[2][4] Nationally, the drop fell short of the nosedive some analysts anticipated.
Premium impacts proved contained for the vast majority. Subsidized enrollees – about 90 percent of the total – faced an average monthly payment of $73 in 2026, comparable to $77 in 2022 before enhancements kicked in.[1]
Cleaning Up Ineligible Enrollments Drove the Dip
Officials attributed much of the enrollment decline to rigorous eligibility checks rather than affordability woes. The CMS terminated subsidies for nearly 1.5 million people deemed ineligible, including those double-enrolled in Medicaid or lacking required income documentation.[1]
Unauthorized enrollments also faced cancellation. These measures addressed fraud and overlaps that swelled prior years’ numbers under looser rules.
- Concurrent Medicaid enrollment: Major factor in terminations.
- Missing prior-year income records: Prevented subsidy continuity.
- Improper special enrollment periods: Curbed opportunistic sign-ups.
- Overall ineligible cases: Approaching 1.5 million nationwide.
| Year | National ACA Enrollment (Millions) |
|---|---|
| 2024 | 16.3 |
| 2025 | 24.3 |
| 2026 | 23.1 |
Shifting Focus in Washington
With no crisis unfolding, Democrats pivoted quickly. Shutdown threats resurfaced over unrelated issues like immigration funding. Critics pointed to repeated tactics eroding public trust.
The episode underscored how pandemic-era boosts inflated expectations. Basic subsidies persist, cushioning costs for lower-income households without the cliff’s sharp edge for others.
In Nevada, the public option’s debut offered locals alternatives amid federal changes, though it fell short of initial targets.[5]
Key Takeaways
- Enrollment declined modestly due to eligibility enforcement, not premium shocks.
- Average subsidized premiums held steady at around $73 monthly.
- Predictions of mass coverage losses did not bear out nationally or in Nevada.
The absence of a subsidy cliff challenges narratives of inevitable ACA turmoil. Stable figures suggest the program’s resilience, even sans enhancements. What do you think about the outcome? Tell us in the comments.